F is for Feeding
/There is so much involved with the different options of how to feed your baby. I will not be able to go into that much detail on this blog post, but if you have specific questions about anything to do with feeding your baby please comment or send me a message and I would be happy to help.
There are essentially three ways you can feed your baby. Breastfeeding, bottle feeding pumped milk, and formula feeding – or any combination of the three. I will present the basic information covering the essentials of each option.
Breastfeeding
In the long run breast feeding your baby will be the cheapest option and most likely the easiest. In the beginning it may be more difficult while you try to help your baby latch properly and figure out the best position for feeding your tiny new baby. But after the first few weeks any discomfort you felt in the beginning should begin to relieve as your baby grows and you both have discovered how to have a proper latch and what positions work best. When settling down to breastfeed your baby, especially in the beginning, it is a good idea to have a snack or two and glass of water close by. Nursing can cause extreme thirst and hunger. Breast feeding provides many additional benefits to you and your baby; it isn’t simply feeding your baby.
Breastfeeding is important for so many reasons. Breastfeeding is beneficial to both your baby’s and your health. Your breastmilk changes as your baby grows and its needs change. The first milk, colostrum, delivers the important nutrients needed for your newborn in a highly concentrated form. Colostrum also helps clear the bowels of meconium and coats your baby’s intestines with a protective layer of enzymes to help prevent gut health issues later on. Breastmilk is unique for each baby and meets their specific needs each time they nurse, changing as needed to fight off any illnesses. Breastmilk has also been shown to reduce your baby’s risk of developing asthma, leukemia, obesity, ear infections, allergies, eczema, diarrhea, vomiting, lower respiratory infections, necrotizing enterocolitis, and SIDS. With almost every potential illness listed the risk of your child developing it decreases the longer you breastfed.
Breastfeeding has many health benefits for you as well. A woman who breastfeeds is said to have a lower risk of developing postpartum mood disorders, osteoporosis, type 2 diabetes, certain types of breast cancer, and ovarian cancer. And most research shows that the longer you breastfeed, over the course of all your children, the lower your risk of developing the diseases. This is thought to decrease your risk of developing cancer because the longer you breastfeed the longer your ovulation cycle is delayed thus lowering your exposure to the hormone estrogen, as estrogen can promote the growth of breast cancer cells. Breastfeeding also sheds breast tissue which increases the chance that cells with potential DNA damage will be shed. In addition, when breastfeeding most mothers eat healthier and give up smoking and drinking which in and of itself leads to a healthier lifestyle and a decreased risk of developing a potential disease.
If you are struggling with establishing a proper latch make sure you consult a lactation consultant in your area to determine if your baby has any lip or tongue ties and to assist you with positioning your baby.
Once you have established a good latch breastfeeding becomes almost effortless and it should never be painful. You never have to worry about if you have formula or clean bottles with you when you go out. And you always have the means to feed your baby in any situation, with or without power and running water. All 50 states finally have laws that protect a woman’s right to breast feed her baby in public; it is up to you when, where, and how you decide to feed your baby.
Bottle Feeding Pumped Milk
Sometimes babies are born too early to breast feed and the mom must pump if she wishes to feed her baby breastmilk. Or maybe you have to go back to work, but still want to feed your baby breastmilk as much as possible. There are also phenomena known as breastfeeding aversion and agitation (BAA) and Dysphoric Milk Ejection Reflex(D-MER) that cause the nursing mother to have negative or angry thoughts, in these situations you may decide to pump instead. Whatever your reason for deciding to pump there are some steps involved in the pumping process and tips for how to feed the bottle to your baby.
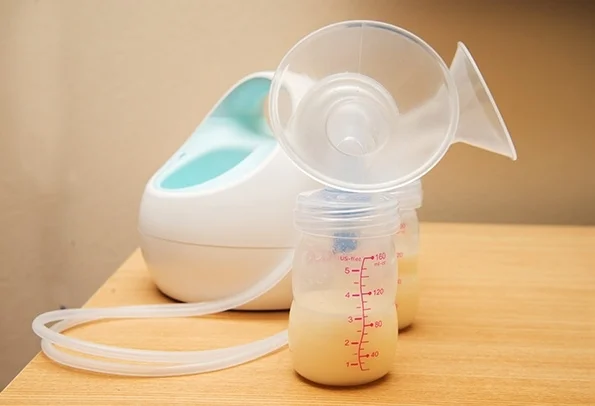
To use a breast pump it is important to read the directions and learn the skills necessary to pump efficiently and effectively. Just like learning to breastfeed initially requires some practice, so does pumping breastmilk. The first step is to determine what pump you would like to use and if you would like a single or double pump and a manual or electric pump. Almost all insurance policies these days should cover at least a basic double electric pump. Double pumping may be more effective for quickly emptying both breasts and stimulating supply. Once you have determined which pump you would like to use the next step is ensuring you have the correct flange size.
Follow the directions for correctly assembling the pump and make sure you have a drink and snack accessible before you begin pumping – especially in the beginning. To start pumping, center the flanges over the nipples and hold in place with your hands or a pumping bra. Start with a light, fast, suction setting until letdown begins at which point you should switch the setting to a longer harder suction. This mimics the way a baby sucks to initiate letdown and then changes their suck to drink the flowing milk. The suction should never be uncomfortable; if it is you should use a lower suction setting or try adjusting the flanges.
The next step is determining when to pump. If you plan on only pumping occasionally you should ensure you at least pump every time you miss a nursing session to ensure your supply is maintained. The best time to pump to have extra milk on hand is in the morning, between 1-6am, as you produce the most milk overnight. If you plan on pumping in between feedings you should pump 30 minutes after your last nursing session and at least an hour before the next session, this ensures you have enough milk to feed your baby with the next nursing session. If your baby insists on nursing right after a pumping session he/she will still get milk, the session may just take longer than usual. If you will be exclusively pumping you want to make sure you pump 9-10 times each day, aiming to pump 30 oz total in a 24 hour period. If pumping will begin immediately after birth you should begin pumping no more than six hours after your baby is born. Remember that your milk supply is based on supply and demand, the longer and more frequently you pump the more milk you will produce.
In between pumping sessions all parts of the pump exposed to milk need to be washed; bottles, flanges, and membranes or duckbills. They should be allowed to air dry to avoid contamination from a dirty towel. To store milk you can store it in plastic bottles, glass bottles, or freezer bags – keeping in mind that milk expands when frozen. Milk can be safely stored at room temperature for 3-8 hours, in the fridge for 3-5 days, in the freezer for 3-9 months, and in the deep freeze for 6-12 months. If there is milk left over after feeding the baby it needs to be used or thrown away in 1-2 hours. Once you thaw milk, it cannot be re-frozen. Milk can be thawed by leaving it in the fridge overnight, running it under warm water, or resting it in warm water – never microwave or shake the milk. Thawed milk should be used within 24 hours.
To wean from the pump you need to gradually decrease the number of pumping sessions or the length of each session. Drop one pumping session every 3-4 days or decrease all pumping sessions by 5 minutes every 3-4 days. This will allow you to safely stop pumping without causing engorgement and risking a clogged duct or mastitis.
When feeding your baby pumped milk you will want to follow paced bottle feeding. This feeding method mimics breastfeeding. Your baby will eat slower and have to work harder using this method than typical bottle feeding. This method of feeding is designed mainly for breastfeeding mothers who need to bottle feed as well, but can be beneficial to those who are only bottle or formula feeding. In the beginning you should use a slow flow or newborn nipple. When pace feeding, you should hold your baby more upright, tickle your baby’s lips to initiate the rooting reflex, insert the nipple into your baby’s mouth when they open, hold the bottle horizontally slowing the flow of milk, and remove the bottle after about 30 seconds; repeat until finished. This pattern mimics breastfeeding, as your baby would naturally suck, swallow, and pause before repeating. Using this method of feeding will extend the length of a feeding session by 5-15 minutes; this allows your baby to learn when he is full because he will get the signals of satiety before his belly is overly full.
The biggest struggle with bottle feeding is determining when your baby is full. Watch for signs such as slower sucking, wandering eyes, falling asleep, or open and relaxed hands.
Read the next section for more information on cleaning your bottles.
Formula Feeding
There are many options you face when formula feeding. In addition to deciding on what type of bottle and nipple to use, you also have to decide on what type of formula. And once you choose a formula you still have to decide between powder, concentrate, or a ready-to-feed style. You may decide to have some of each on hand to determine which works best for you in everyday situations and to have the ready-to-feed option in case of a water outage or middle of the night feedings to save some time.
When deciding on a type of formula you should choose one that is iron-fortified and consider any family allergies or intolerances – such as dairy. Otherwise most formula is basically the same; they are all mandated by the FDA to include 29 essential nutrients in each serving. DHA however is not required, so you may want to consider a formula that has added this.
Before feeding your baby, make sure your bottle, nipple, and any other bottle components have been cleaned. Most packaging recommends sterilizing or at least cleaning all components with soap and warm water before use. Some doctors recommend you sterilize your bottle components before each use, at a minimum they need to be thoroughly washed and air dried between each use.
To prepare the formula, follow the package directions exactly. Never add extra water or extra formula. Too much water will prevent your baby from getting all the calories and nutrients he/she needs, and too much formula can cause dehydration and constipation. It is recommended that you use boiled water to mix your formula to ensure all bacteria have been killed, especially if you are unsure about your water quality. Once you prepare the formula you should use or refrigerate the bottle within one hour. Once refrigerated you need to use the formula within 24 hours. Most baby’s prefer warm milk, but you can feed your baby formula straight from the fridge without warming it. To heat up the formula, the easiest way is to place the bottle in a pan of water on the stove or use a bottle warmer. Never microwave the milk as it can cause pockets of extremely hot and cold milk in the bottle. To make sure your bottle is the right temperate place a few drops from the bottle on the inside of your wrist.
You should not add sugar or cereal to a bottle as this can cause an upset stomach and other possible issues.
Never feed your baby lying down as the milk can pool in the middle ear and cause an infection. Make sure you don’t over feed your baby – this is easy to do the first week. On the first day, your baby’s stomach is about the size of a cherry, or 5-7ml. By day three, your baby’s stomach is about the size of a walnut, or 22-27 ml. At one week of age your baby’s stomach will be the size of an apricot or about 2 oz. After the first week of life you can begin giving your baby more milk in his/her bottles, about 2-4 ounces per feeding every two to four hours. Follow your baby’s hunger cues, as it is best to feed your baby on demand. Never force your baby to finish a bottle, and if your baby still seems to want to suck after the bottle is empty you can offer him/her a little more. Whatever milk your baby does not finish from the bottle should be thrown away. If you premix formula to use, only put what you think your baby will eat in that feeding session in the bottle, once exposed to your baby’s saliva, bacteria can grow in the milk.
For more detailed information on how much to feed your baby as they grow here is a great article from Baby Center.
Babies digest formula more slowly than breastmilk, so if you are switching from breastmilk to formula, or supplementing occasionally with formula, keep this in mind. If supplementing, make sure you note what time of day the formula was given and know that your baby may not be ready to eat again when he/she usually is.
If your baby seems to gulp a lot of air when eating, you will want to burp your baby after every two to three ounces, even if this means you have to burp them in the middle of a feeding. You can burp your baby draped over your shoulder, sitting upright on your lap, or laying down on his/her stomach on your lap.
There are many options when it comes to feeding your baby, and while breastmilk is known to be the most nutritional option, it may not be the best option for you. If you or your baby feel breastfeeding isn’t right for you then pumping or feeding formula is going to be what is best for you. Forcing yourself to feed your baby a certain way due to pressure from friends or family could lead to resentment and negative feelings, disrupting your ability to bond with your baby.
Do you have any helpful tips that helped you breastfeed, pump, or formula feed?
Next week I will be blogging on the letter G… G is for Gas.